Endometriosis is a condition in which endometrium, the tissue that normally lines the interior of your uterus, grows outside your uterus. It is a painful condition. The tissue lining your pelvic, fallopian tubes, and ovaries are all frequently affected by endometriosis. Occasionally, tissue resembling endometrium may be seen outside the region around the pelvic organs.
Endometrial-like tissue that has endometriosis behaves like endometrial tissue would: it swells, degrades, and bleeds with each menstrual cycle. Yet, this tissue becomes stuck since it has nowhere to go but inside your body. Endometriomas, or endometrial cysts, can develop when endometriosis affects the ovaries. Scar tissue and adhesions, bands of fibrous tissue can cause pelvic tissues and organs to attach to one another and can form when nearby tissue becomes irritated.
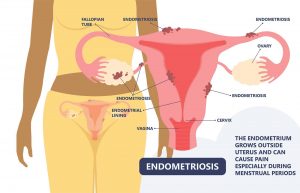
Pain from endometriosis, which can occasionally be severe, is common, especially during menstruation. Moreover, fertility issues could arise. Thankfully, there are solutions that work.
Symptoms
The main sign of endometriosis is pelvic pain, which is frequently related to menstruation. Although many women suffer cramps throughout their periods, individuals who have endometriosis frequently have significantly more severe menstrual pain than usual. With time, pain may potentially get worse.
The following are typical endometriosis symptoms and signs:
Painful periods (dysmenorrhea): Before and for a few days after a period, pelvic pain and cramps are common. Furthermore, lower back and stomach ache are possible.
Discomfort during sexual activity: Endometriosis often causes pain during or after sex.
Discomfort when urinating or using the restroom. These symptoms are most likely to occur during a menstrual period.
Excessive bleeding: Periodically, you might have thick periods or bleed between periods (intermenstrual bleeding).
Infertility: When a person seeks therapy for infertility, endometriosis is occasionally discovered for the first time.
Additional symptoms and indicators. Especially during menstrual periods, you can have tiredness, diarrhoea, constipation, bloating, or nausea.
Your condition’s severity may not always be accurately predicted by how much pain you are in. Endometriosis can be moderate and cause considerable pain, or it can be advanced and cause little to no pain.
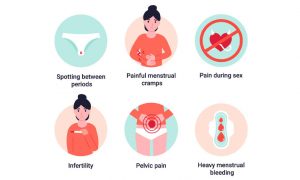
Endometriosis Symptoms
Endometriosis is commonly mistaken for other medical disorders, such as pelvic inflammatory disease (PID) or ovarian cysts, that can also cause pelvic pain. It could be mistaken for irritable bowel syndrome (IBS), which also produces stomach cramping, constipation, and episodes of diarrhea. Endometriosis and IBS can coexist, which makes a diagnosis more difficult.
Whenever to visit a doctor
If you experience any symptoms or indicators that could point to endometriosis, consult your doctor.
The condition of endometriosis might be difficult to control. Better symptom treatment may be achieved with an early diagnosis, a multidisciplinary medical team, and comprehension of your diagnosis.
Causes
Although the precise cause of endometriosis is unknown, the following factors may contribute:
Retrograde menstruation: Menstrual blood with endometrial cells flows back through the fallopian tubes and into the pelvic cavity during retrograde menstruation, as opposed to leaving the body. These endometrial cells adhere to the surfaces of the pelvic organs and pelvic walls, where they develop throughout each menstrual cycle, thickening, and bleeding.
Peritoneal cell transformation. According to the “induction theory,” which has been put out by researchers, hormones or immunological factors encourage peritoneal cells, which line the inside of your belly, to change into endometrial-like cells.
Transformation of embryonic cells: During puberty, hormones like estrogen may cause embryonic cells, which are still in the early stages of development, to grow into endometrial-like cell implants.
Implanting a scar following surgery. Endometrial cells may adhere to an incision following surgery, such as a hysterectomy or C-section.
Transport of endometrial cells. Endometrial cells may be transported to different areas of the body through blood vessels or the tissue fluid (lymphatic) system.
An immune system condition. The body may not be able to recognize and eliminate endometrial-like tissue that is developing outside the uterus if there is a problem with the immune system.
Risk concerns
You are more likely to get endometriosis if you have certain conditions, like:
Never having children
Having your first menstruation at a young age
Having a later onset of menopause
Shorter than 27 day menstrual cycles
Heavy, longer-than-seven-day menstrual periods
Having more estrogen in your system or being exposed to more of the estrogen your body produces over the course of your lifetime
A low body mass index
Endometriosis in one or more family members (mother, aunt, or sister)
Any medical ailment that interferes with the body’s ability to expel blood during menstruation
Issues with the reproductive system
Often, endometriosis appears several years after the start of menstruation (menarche). If you are not taking estrogen, endometriosis signs and symptoms may only slightly improve during pregnancy and totally disappear at menopause.
Complications
Infertility: Impaired fertility is the main problem of endometriosis. Between one-third and fifty percent of endometriosis, patients struggle to conceive.
An egg must be released from an ovary, pass via a nearby fallopian tube, be fertilized by a sperm cell, and then adhere to the uterine wall to start developing in order for pregnancy to occur. The tube may become blocked by endometriosis, preventing the egg and sperm from merging. Yet, the illness also appears to have indirect effects on fertility, such as harming sperm or eggs.
Nonetheless, many people with mild to moderate endometriosis are nevertheless able to become pregnant and carry it to term. Endometriosis patients are occasionally advised by doctors to not delay starting a family because the condition could get worse with time.







